Drug treatments for obesity
Current drug treatments for obesity are relatively ineffective. Whilst many treatments are successful in promoting weight loss in the short term; long term maintenance is a key problem that has yet to be overcome. With the ever inceasing prevalence of obesity in the developed, and now developing world, it is an integral concern to epidemiologists, policy makers and scientists looking to treat obesity. Here we explain the basic mechanisms of action underlying the current pharmacological treatments and also the avenues of development that any future drugs may take.
Serotonin & Noradrenaline Related Drugs
Many drugs reduce appetite by activating serotonin 5-HT2C receptors. This may occur via:
- Nonselective activation of multiple biogenic monoamines by reuptake inhibition. Sibutramine and tesofensine[1] have this mechanism.
- Selective agonism of serotonin 5-HT2C receptors by drugs such as lorcaserin decreases appetite via the proopiomelanocortin system.[2]
Sibutramine was originally used in the treatment of depression [3] but is now used to help overweight patients lose weight, and along with Orlistat, in 2008 was the only drug licensed for such use in the UK. [4] It acts within the hypothalamus by preventing reuptake of both noradrenaline and serotonin. [5][6] This produces increased feelings of satiety, a decreased appetite, and a lower intake of food which results in weight loss. [7] Some studies have shown that sibutramine may increase thermogenesis and as such, contribute to weight loss, but in other studies no such effects were shown, and it seems that this action contributes in, at most a minor way to weight loss. It is also thought that sibutramine may effect levels of the hormones leptin and ghrelin, as well as central neuropeptide Y (NPY), and proopiomelanocortin (POMC) mRNA. Sibutramine treatment differs to orlistat in relation to leptin, as, when using sibutramine, transfer of leptin into the brain is maintained or even increased during weight loss which does not happen when using orlistat.
A major side-effect of sibutramine therapy is a dose-dependent increase of both blood pressure and heart rate, and as obese patients are likely to already have elevated blood pressure and heart rate, it is important to check these regularly in obese patients taking sibutramine. Patients with hypertension and/or cardiovascular disease are strongly advised against taking the drug. Sibutramine can also on occasion cause the patient to suffer from a dry mouth, constipation and insomnia. [8] Adolescents taking sibutramine should be regularly checked for a possible increase in suicidal thoughts, as it acts in a similar way to anti-depressants by preventing noradrenaline and serotonin uptake. [5]
This drug has now been withdrawn in the UK for fears of it increasing the likelihood of heart attacks and strokes
Endocannabinoids
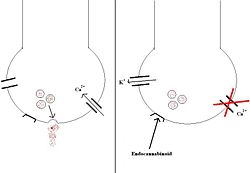
Endocannabinoids are substances produced within the body, including in the brain itself, that mimic the effects of cannabis, and cannabis has long been known to stimulate appetite. Endocannabinoids act on very specific cannabinoid receptors, of which there are two types: CB1 receptors, which are mainly found within the central nervous system (mainly on presynaptic nerve endings), and CB2 receptors, which atre mainly found in peripheral tissues. CB1 receptors are G-protein coupled receptors, located on the plasma membranes of neurones in specific regions of the brain, including the hypothalamus and in the brain's 'reward' pathways. When a cannabinoid agonist binds to the CB1 receptor on a neurone, it has two main actions: 1) calcium entry to the cell is inhibited 2) potassium channels are activated, causing the neurone to become hyperpolarised. The overall effect is that neurotransmitter release from that neurone is inhibited.
Rimonabant
CB1 receptor antagonists, in particular rimonabant, have been used to treat obesity. The link between appetite and CB1 receptors is unclear, but is likely to involve CB1 receptors in the hypothalamus. Mice genetically engineered to be deficient in CB-1 receptors are resistant to diet-induced obesity, and clinical trials of rimonabant have demonstrated significant weight loss in obese subjects when combined with a reduction in calorie intake, as well as an improvement the ratio of "good" (HDL) to "bad" (LDL) cholesterol.[9] The weight loss, however, extends beyond the transient decrease in appetite. In candy-fed animals, rimonabant increased the amount of fat available for combustion after a meal, and that this was not an indirect, compensatory, consequence of food deprivation, but a direct neuroendocrine effect.[10] It is now known that blocking type 1 cannabinoid receptors triggers the birth of new mitochondria (the fat-burning power plants of the cells) in adipocytes,[11] obviously a beneficial effect for weight loss.
A problem with using CB1 antagonists is the incidence of psychiatric problems, in particular, depression; several suicides occurred during clinical trials. [5] As a result, the FDA has not approved the use of rimonabant in the USA. The European Medicines Agency (EMEA) has recommended the marketing authorisation of rimonabant be suspended across the EU, and consequently the National Institute for Health and Clinical Excellence (NICE) has withdrawn its guidance for the use of the drug.[12]
Peripheral Drugs
Orlistat
‘Peripherally acting anti-obesity drugs’ work by reducing the calorie intake from food, or by altering the metabolism of it in the gastrointestinal system (gut). Currently only one drug of this kind is approved for use globally - Orlistat (Xenicol), and it works by inhibiting the enzyme lipase that breaks down fat in the gut, meaning that the fat cannot be absorbed from food, and instead it is excreted out of the body. [13] This can reduce the amount of fat absorbed from the gut by 30%, causing a decreased calorie intake and therefore weight loss. The weight loss from taking this medication is between 5-10% on average. [14] Orlistat also improves several other cardiovascular risk-factors. Low-density lipoproteins (LDL) and triglyceride levels were reduced by more than expected for the weight loss, as well as blood pressure, waist circumference and lipids being reduced. [15] Some research also suggests that Orlistat reduces fasting glucose and HbA1c levels in type 2 diabetics by more than predicted for the weight loss, with suggested methods including increased insulin sensitivity and glucagon-like peptide-1 secretion in the small intestine. Orlistat also reduces the risk of type 2 diabetes in obese subjects. [7]
However, this drug has side-effects. Oily-spotting, flatulence, abdominal cramps, faecal urgency/incontinence and liquid stools are the common adverse effects, due to an increase of fat in the gut and stools. [13] These side-effects are reported to only be experienced during the early stages, and subside as patients learn to use the drug. [5] Orlistat also prevents some absorption of fat-soluble vitamins (vitamins A,E,D and K), and so patients are recommended to take supplements. The drug does not have any systemic side-effects as it is contained in the gut, but it does affect the absorption of acyclovir (an antiviral), so they shouldn’t be used at the same time. [5]
In 2001 the National Institute for Health and Clinical Excellence (NICE) issued a press release on guidance for Orlistat use, and it states that it is cost effective to the NHS. [16]
Gut hormones
As well as drugs that work in the periphery to cause weight loss, some hormones produced in the body cause satiety. One example is amylin, which is a hormone secreted along with insulin from the pancreas in response to a meal, causing you to feel full, therefore regulating your meal size. An amylin analogue, Pramlintide, is currently being looked into as a potential anti-obesity therapy, and is already being used in diabetics. [15]
Glucagon-like peptide-1 is released from the gut during eating, and relays satiety information to the brain via the vagus nerve. [15] Liraglutide is a long-acting analogue of glucagon-like peptide-1 and has recently been shown to be effective in non-diabetic groups[17], resulting in significant weight loss compared to a placebo and orlistat. Liraglutide also reduced fasting lipids and mean systolic blood pressure. With regard to long-term weight maintenance, further studies are still required.
Peptide YY, also released from the gut, could also be a potential for use, along with pancreatic polypeptide (PP) – both of which decrease appetite. Small-scale trials in a peptide called Oxyntomodulin have also been promising, with larger trials waiting to be preformed. [15]
Other Drug Therapies
Some drugs are not primarily indicated for use as weight loss therapies but may be effective in this role.
Metformin & Acarbose
In patients with type II diabetes, there is evidence to support the use of metformin and acarbose as weight loss agents. [18] The role of metformin in stabilising blood glucose levels has been shown to aid weight loss and also - perhaps by another mechanism - to reduce appetite. [19] Acarbose is believed to simply slow nutrient digestion and interact with glucagon-like peptide-1 to aid a slight weight loss. In contrast, patients without type II diabetes will not benefit to the same extent although trials have shown minor improvements. [14] In The Diabetes Prevention Program, the weight loss achieved in a group of non-diabetic patients taking metformin was approximately half of that of a 'lifestyle modification' group, and the mean weight loss was only slightly higher than in the placebo group. [20]. Acarbose is of even less use in this context, neither helping with weight loss or with maintaining a healthy weight.
Diuretics
Diuretics, cause an increase in fluid loss (e.g. by means of hypo-absorption in the nephron), and as such have no role in weight loss by reducing body fat stores. They are abused, however as means of a 'quick-fix' pseudo-weight loss, giving the impression of a reduction in body weight whilst in reality, they are simply causing dehydration. They have been used for some time in the sporting world, particularly boxing, for boxers to 'make the weight' or simply to reduce likelihood of other drugs being found by urine testing. [21] They are also used by women suffering from pre-menstrual water retention. [22]
Thyroid Hormones
One potential method of tackling obesity is the use of thyroid hormone mimetics. Thyroid hormones (T3, T4) act on the thyroid hormone receptors (THR) to elevate the body’s metabolic rate, increasing oxygen consumption leading to an increased use of fat for energy production. However the hormones also have stimulatory effects on the heart rate, causing tachycardia and dangerous arrhythmias, as well as raising the metabolism of muscle protein and promoting bone turnover. [23]
Thyroid hormone mimetics – compounds with similar effects on the fat metabolism without causing any of the unwanted cardiac symptoms – have been developed and tested on animals. One of these named GC-1, an agonist for the thyroid hormone receptor beta 1 (THRB1) has been shown to have minimal effects on the cardiac muscle, whilst stimulating fat metabolism in rats. GC-1 has also been shown to reduce body weight in primates, though this may not specifically be fat loss.
GC-1 and KB2155 (another THRB1 agonist) have been tested in human trials, with no report of weight loss, though this could be due to insufficient doses or the minimal trial period. It remains to be seen what benefit these drugs could offer in humans, both on obesity and on other metabolic conditions. [24]
Caffeine & Ephedrine
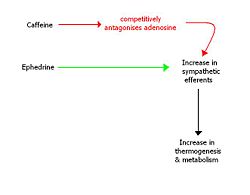
Caffeine is a stimulant belonging to the xanthine class of drugs. It is an attractive pharmacological agent for consideration in the context of helping people to lose weight, not only because of its wide global availability, social acceptability and price. Caffeine increases thermogenesis in humans and reduces appetite, but is less effective as a long-term weight loss agent. [25] This is believed to be because of the tolerance (upregulation of adenosine receptors) that develops to caffeine usage.
Ephedrine is a sympathomimetic amine, which acts as a stimulant and appetite suppressant. It has mild efficacy as a weight loss drug and when combined with caffeine, can be very effective for long-term weight loss. [26] However, there are problems associated with the fact that both drugs act to increase the outputs of the sympathetic nervous system; these include a rise in blood pressure, palpitations, insomnia and tremor.
Efficacy
A systematic review found that the average weight loss after at least one year was:[27]
- Orlistat: 2.9 kg, but with gastrointestinal side effects.
- Sibutramine: 4.2 kg, but with raised blood pressure and pulse.
- Rimonabant: 4.7-kg, but associated with increased psychiatric disorders. About a third of patients discontinued treatment.[28][27]
Subsequent trials show:
- Tesofensine may be effective[29]
- Lorcaserin may be effective[30]
References
- ↑ Astrup A et al. (2008). "Effect of tesofensine on bodyweight loss, body composition, and quality of life in obese patients: a randomised, double-blind, placebo-controlled trial". Lancet 372: 1906–13. PMID 18950853.
- ↑ Smith SR, Weissman NJ, Anderson CM, Sanchez M, Chuang E, Stubbe S et al. (2010). "Multicenter, placebo-controlled trial of lorcaserin for weight management.". N Engl J Med 363 (3): 245-56. DOI:10.1056/NEJMoa0909809. PMID 20647200. Research Blogging.
- ↑ Woo T (2009) Pharmacotherapy and surgery treatment for the severely obese adolescent. J Paediatric Health Care 23:206-12
- ↑ Rang H et al.(2007) Pharmacology. Churchill Livingstone, Elsevier. 417-8
- ↑ Jump up to: 5.0 5.1 5.2 5.3 5.4 Bray G (2008) Lifestyle and pharmacological approaches to weight loss: efficacy and safety. J Clin Endocrinol Metab 93:S81–8
- ↑ Tziomalos K et al. (2009) The use of sibutramine in the management of obesity and related disorders: An update Vascular Health and Risk Management 5:441-52
- ↑ Jump up to: 7.0 7.1 Coutinho W (2009) The first decade of sibutramine and orlistat: a reappraisal of their expanding roles in the treatment of obesity and associated conditions. Arquivos Brasileiros Endocrinol Metabol 53:262-70
- ↑ Boon NA et al.(2006) Davidson's Principles & Practice of Medicine 111-7
- ↑ Kintscher U (2008) The cardiometabolic drug rimonabant: after 2 years of RIO-Europe and STRADIVARIUS Eur Heart J
- ↑ Herling AW et al. (2008). "Increased energy expenditure contributes more to the body weight-reducing effect of rimonabant than reduced food intake in candy-fed wistar rats". Endocrinology 149: 2557–66. DOI:10.1210/en.2007-1515. PMID 18276749. Research Blogging.
- ↑ Tedesco L et al. (2008). "Cannabinoid type 1 receptor blockade promotes mitochondrial biogenesis through eNOS expression in white adipocytes". Diabetes. DOI:10.2337/db07-1623. PMID 18477809. Research Blogging.
- ↑ NHS National Institute for Health and Clinical Excellence: Guidance: Obesity - rimonabant (withdrawn) (2008), Available http://www.nice.org.uk/TA144
- ↑ Jump up to: 13.0 13.1 Elangbam CS (2009) Current strategies in the development of anti-obesity drugs and their safety concerns. Vet Pathol 26:10-24
- ↑ Jump up to: 14.0 14.1 Desilets AR et al.(2008) Role of metformin for weight management in patients without type 2 diabetes Ann Pharmacotherapy 42:817-26
- ↑ Jump up to: 15.0 15.1 15.2 15.3 Zanella M, Filho F (2009) Emerging drugs for obesity therapy Arq Bras Endocrinol Metab 53:271-80
- ↑ NHS National Institute for Health and Clinical Excellence: Press release (2001), Viewed 7 October 2009,
- ↑ Astrup A et al. (2009). "Effects of liraglutide in the treatment of obesity: a randomised, double-blind, placebo-controlled study". Lancet 374: 1606-16. DOI:10.1016/S0140-6736(09)61375-1. PMID 19853906. Research Blogging.
- ↑ Siraj ES] (2003) Is there a role for metformin or acarbose as a weight-loss agent in the absence of diabetes? Cleve Clin J Med 70:702-4
- ↑ Hauptman J et al. (2000) Orlistat in the Long-term Treatment of Obesity in Primary Care Settings. Arch Fam Med 9:160–7
- ↑ Knowler WC et al. (2002) Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 346:393-403
- ↑ Bulik CM (1992). Abuse of drugs associated with eating disorders. J Subst Abuse 4:69-90.
- ↑ Wagner JC (1991). Enhancement of athletic performance with drugs. An overview. Sports Med 12:250-65
- ↑ Rang H et al. (2007) Pharmacology. Churchill Livingstone, Elsevier. pp 441-4
- ↑ Baxter JD, Webb P (2009) Thyroid hormone mimetics: potential applications in atherosclerosis, obesity and type 2 diabetes. Nat Rev Drug Discov 8:308-20l
- ↑ Greenway FL (2001) The safety and efficacy of pharmaceutical and herbal caffeine and ephedrine use as a weight loss agent. Obes Rev 2:199-211.
- ↑ Diepvens K et al.(2007) Obesity and thermogenesis related to the consumption of caffeine, ephedrine, capsaicin, and green tea Am J Physiol 292:R77-85
- ↑ Jump up to: 27.0 27.1 Rucker D et al. (2007). "Long term pharmacotherapy for obesity and overweight: updated meta-analysis". BMJ. DOI:10.1136/bmj.39385.413113.25. PMID 18006966. Research Blogging.
- ↑ Christensen R et al. (2007). "Efficacy and safety of the weight-loss drug rimonabant: a meta-analysis of randomised trials". Lancet 370: 1706–13. PMID 18022033.
- ↑ Astrup A et al. (2008). "Effect of tesofensine on bodyweight loss, body composition, and quality of life in obese patients: a randomised, double-blind, placebo-controlled trial". Lancet 372: 1906–13. PMID 18950853.
- ↑ Smith, SR; et al. (2010-07-15). "Multicenter, placebo-controlled trial of Lorcaserin for weight management". N Engl J Med 363: 245-56. Retrieved on 2010-07-15.