Poverty and obesity
Poverty and obesity are closely linked, but the relationship is complex. Whilst historically being overweight was predominantly seen in the upper class as a sign of wealth and prestige, recent trends show a somewhat different picture. In the USA, some of the highest rates of obesity occur in the poorest population groups and in the UK the trends are similar. The inequality in income resulting in obesity is largely associated with less expenditure on food, decreased diet quality, and energy-dense foods that represent the lowest-cost option for consumers. Cheap palatable foods high in fat, sugar and energy are the result of developments in agriculture and food technology and the shifting ‘nutrition transitition’ now seen in developing countries highlights the need for a greater awareness of diet quality and a need for preventative action to hinder the growing obesity epidemic in both high income and low income areas. [1]
Diet Quality
The Relationship Between Diet Quality and Socio-Economic Status
Eating a high quality diet helps to maintain good health. This involves consuming an appropriate balance of essential nutrients, macronutrients, calories and water from different foods[2]. Some nutrients are required in a greater supply than others, and the dietary needs of each individual vary with their body composition, basal metabolism and daily activity levels.
The World Health Organisation and national government schemes have been active in publicising healthy eating guidelines to educate people in how to have a high quality diet. However, there are still many individuals with low quality diets. Such poor diets often involve excessive calorie intake and consist of too much fat, sugar and salt. Bad diet quality can be detrimental to general health by contributing to many health risks such as obesity, hypertension, heart disease, diabetes and cancer[2]. People with low socio-economic status (low income families or poorly educated individuals) have poorer quality diets and tend to be more obese than people of high socio-economic status[2].
Evidence for Socio-Economic Status Affecting Diet Quality
Many studies have investigated how different aspects of the diet are consumed in high-income and low-income families, and have found that the consumption of different food types is unevenly distributed across the socio-economic gradient[2].
Fruits and vegetables provide a natural source of essential nutrients that are considered to be a vital part of good quality diet. Families of high socio-economic status are more likely to eat higher quantities of fresh fruits and vegetables, and also eat a greater variety of these foods[3]. Data from the USA, Canada, the UK, many countries in Europe, and Australia provide strong evidence that those with higher socio-economic status eat more fruits and vegetables than those individuals with a lower income and education[3][4][5].
Protein is an important component of a healthy diet and different socio-economic groups generally eat different food products to obtain protein. Those with low socio-economic status tend to eat more fatty meats and less fish. Meat and fish that is consumed by this group tends to be canned, breaded or fried[6]. These products have a lower nutritional value and can be high in calories and fat. Lean meats and fish, including other seafood, is mostly consumed by those of high socio-economic status[7]. These food products are considered to be healthier, and good quality fish products are essential for omega 3 intake in the diet.
Sweets consumption is similar as far as quantity is concerned across the socio-economic gradient. However, low socio-economic status is associated with a greater intake of sugar from sweetened beverages and ready meals with added sugar[7]. Low socio-economic status is also associated with a greater consumption of foods with added fats[6].
Causation of Poor Diet Quality in People of Low Socio-Economic Status
Socio-economic status is largely determined by income. Low-income individuals are limited in what foods they can afford, and will generally choose food items that will satisfy hunger at the lowest cost. The cheapest foods in supermarkets tend to be nutritionally deficient and high in calories, fats and sugars which, when eaten in large amounts, contribute to health issues such as obesity[2].
Healthy foods that are high in vitamins and nutrients such as fruits, vegetables, nuts and whole grain breads and cereals tend to be expensive and therefore more affordable to only those of high socio-economic status[8]. Individuals of low income are also inclined to buy dry, packaged foods with a long shelf life that can be stored for longer without the risk of spoiling. These foods generally tend to be of a low nutritional value[9]. This category often buy the same cheap foods every week resulting in an unvaried, monotonous diet. This could be due to wanting to avoid the risk of waste by trying new foods[2].
Another contributory reason for people of low income having poor diet quality could be due to difficulty in accessing supermarkets. Grocery stores and large supermarkets tend to be situated in areas where there are plenty of high income families close to visit the store and buy the products. Individuals of low socio-economic status are less likely to have cars [2]. Studies in the USA have shown that, even within low income populations, if there is a well-stocked supermarket nearby people tend to eat more fruits and vegetables than people of the same income category living in a neighbourhood that has limited access to food[10].
Some studies have suggested that low socio-economic status is associated with a lack of cooking skills and a disinterest in cooking. However, there is little evidence to back up this claim, as there are also correlations between high socio-economic status and limited time for cooking and therefore the preparation of quick and easy to make meals[2].
Obesity occurring as a result of poor diet quality has been correlated with low socio-economic status in the lack of education and motivation. Research has showed that disadvantaged people tend to have a poor knowledge of what foods are nutritionally good for them and have also been shown to be apathetic towards government schemes to promote healthy eating[11]. People in this category tend to have an inaccurate perception of healthy body weight compared to those of better education and income[11].
Therefore, the causation of obesity due to diet quality is multi-factorial and heavily dependent on income and social status. To better target the increasing problem of obesity, healthy eating advice, schemes and help should be given specifically to those of low socio-economic status and other vulnerable groups to promote better diet quality[2].
Dietary Energy Density
Influence on energy intakes
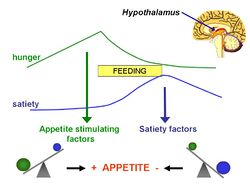
Energy-dense foods result in higher energy intakes overall. Upon eating any given meal under laboratory conditions, participants consume a constant volume. Therefore, the calorie intake is determined by the energy density of the food eaten. In addition, palatable, energy-dense foods have been linked to an attenuation of satiety and ‘passive consumption’, resulting in a greater energy intake [12]. Foods with a low energy density, however, give a lasting feeling of satiety and fullness. This results in a lower consumption of energy during the meal, and for the rest of that day [13]. Studies suggest that the effect of energy density of foods on energy intake is due to poor human ability to distinguish between high and low energy dense foods. Therefore we do not accommodate for this in our eating habits, thus fail to maintain energy balance [14].
Function of water content
The energy density of foods (MJ/kg) is determined by their water content, whereby energy-dilute foods are well hydrated, and energy-dense foods are relatively dry. Energy-dense foods may also contain fat, sugar and starch, and include foodstuffs such as crisps, with an energy density of 23MJ/kg and chocolate (22MJ/kg). Examples of foods with a low energy density are fruits and vegetables [15].
Palatability of energy dense foods
Energy-dense foods tend to be more palatable and pleasurable to eat than foods with a low energy density. Animal studies have shown that sugar and fat stimulate reward centres in brain, resulting in taste preference. It has been proposed that humans, and other animals, developed a taste preference for energy dense foods in order to promote their survival in an environment where food can be scarce and unreliable[16]. Conversely, it has also been suggested that human taste preference for energy-dense foods is acquired during early life. This preference can be developed through repeated exposure, an association with the metabolic consequences, or parental influence[17].
Energy Costs
The Relationship Between Energy Density and Energy Cost
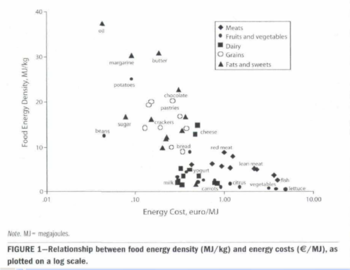
There is an apparent inverse relationship between the energy density of foods and the energy cost of food [18]. This means that energy dense foods are cheaper for food consumption than the healthier less energy dense food substances [19]. The use of refined grains, adding fats and sugars to foods are some of the lowest-cost methods of obtaining energy from our diet [18]. Due to this inverse relationship it is now thought as a way to save money but still have the ability to satisfy the need for food. According to Drewnowski et al. foods such as oil, sugar, potatoes and beans are significantly cheaper than foods such as meat, fish and vegetables for the equivocal overall energy. Figure 1 shows that when applied to a logarithmic scale the difference in energy cost between fresh produce and fats saw a 1000% variation [19]
A French study published in 2004 revealed that for every supplementary 100g portion of fruit and vegetable there was an increase in dietary cost within the range of 0.18 – 0.29 Euros per day. The opposite was seen when an additional 100g of fats or sweets were consumed and an observed 0.05 – 0.40 Euro per day reduction in expenditure was the result [19]).
With the above data being taken from France where the obesity percentage for the population is 9.4%, you can’t help but think the effects of this relationship between energy density and energy cost when put into the context of the UK and USA where obesity percentages are 23% and 30.6% respectively.
Furthermore, recent research suggests that the obesity epidemic in America is now an economic issue, rather than a medical, education or genetic issue. This can be attributed to reasons such as the ‘falling value of the minimum wage’ and an ever present, especially in the populations that categorise into the lower SES’s, a lack of health and family benefits [18].
Ross McEwan 17:05, 14 November 2011 (UTC)
Pricing of Foods and Influence of Income/SES
Fats and sugars provide dietary energy at a very low relative cost. Price reduction studies have been carried out on alternative foods, to investigate whether a reduction in price would see an increase in the consumption of foods such as lower fat foods and fresh fruits. Price reductions of 10%, 25% and 50% applied to lower fat foods resulted in an increase in sales of 9%, 39% and 93% respectively. A second study carried out by the same group showed that reducing the price of fresh fruit and baby carrots by 50% led to a four-fold and two-fold increase in the sale of the products respectively [20].
In a variation of the above study, an increase on high sugar/fat foods price caused a reduction in consumption of such foods. A 20% increase in the price of soda was associated with a 25% decrease in visits to a fast food restaurant per week [21]. This can then be further enhanced into a larger context and if taxes were applied to such foods would we see any significant change in BMI or obesity prevalence across the population [22]. We may see a reduction in the consumption but does this directly relate to a decrease in weight[23] ? Or would this intervention be considered insignificant? [21].Thus, is this observed choice to eat unhealthily that is seen in lower socioeconomic groups due to economic constraints [24]? Darmon et al. highlighted that, when cost restrictions were imposed on individuals not belonging to the lower SES groups, a reduced intake of fruits and vegetables, lean meat etc and an increase in consumption of cereals, fats and sweets was observed. This, being the pattern seen in communities of the lower SES [24].
Ross McEwan 17:10, 14 November 2011 (UTC)
Discussion
For the most part, limited economic resources may shift dietary choices towards an energy-dense, highly palatable diet that involves a high amount of calories per the least volume and ultimately, the least cost. These diets are most likely to contain added sugars and vegetable fats and those from a low socioeconomic status are the most at risk. In addition, poverty has been linked to lower physical activity, lack of nutritional education, poorer access to healthcare, greater exposure to marketing of unhealthy foods, and high stress levels. The appropriate built environment allows the individual adequate access to gyms, parks and healthy food options as opposed to an area with an abundance of fast food restaurants and limited recreational facilities. In many cases, poorer areas are most closely situated to clusters of fast food eateries where there is a lack of healthy choice. Often, in unsafe neighbourhoods there is also a tendency to avoid outdoor activity. Some studies even suggest that those living in high poverty areas are more likely to watch TV.
Overall, research linking poverty and obesity is more consistent for women and children than men of low socioeconomic status but the research has shown varied results in regards to ethnicity and general trends over the last few decades. The CDC in the USA highlight that obesity is higher in minority groups (with the exception of Asian-Americans). In non-hispanic white women, obesity was found to increase as income decreased, whereas in non-hispanic black and Mexican-American men, obesity decreased as income increased. Although the prevalence of obesity among women with income below the poverty level is higher than among those with higher incomes, most obese women do not have incomes below the poverty level.
General obesity trends have shown that, between 1986-2002, BMI was increasingly higher in low income groups than in high income groups, and recently, salary was found to be inversely related to BMI and obesity. However, in one national study spanning 30 years, the relationship between poverty and obesity weakened among most gender and ethnic groups and especially among women, even though overall obesity prevalence increased considerably. Additionally, in some studies obesity rates were found to increase in all income groups; for instance, between 1992 and 2008, obesity prevalence increased by 42.3 percent for the lower income group compared to 88.5 percent for the higher income group. This may suggest that the gaps between low and high income groups may be closing over time as more of the higher income population become obese. Yet some may argue that being poor gives you a very unfair disadvantage. Drewonski
References
- ↑ Drewnowski A, Specter SE (2004) Poverty and obesity: the role of energy density and energy costs Am J Clin Nutr 79:6-16 PMID 14684391
- ↑ Jump up to: 2.0 2.1 2.2 2.3 2.4 2.5 2.6 2.7 2.8 Darmon N, Drewnowski A (2008) Does social class predict diet quality? Am J Clin Nutr 87:1107-1117.
- ↑ Jump up to: 3.0 3.1 Giskes K et al. (2002) Socio-economic differences in fruit and vegetable consumption among Australian adolescents and adults. Public Health Nutrition 5:663–9
- ↑ Irala-Estevez JD et al. (2000) A systematic review of socio-economic differences in food habits in Europe: consumption of fruit and vegetables Eur J Clin Nutr 54:706–714.
- ↑ Ricciuto LE, Tarasuk VS (2007) An examination of income-related disparities in the nutritional quality of food selections among Canadian households from 1986–2001 Social Science and Medicine 64:186–98
- ↑ Jump up to: 6.0 6.1 Johansson L et al. (1999) Healthy dietary habits in relation to social determinants and lifestyle factors Brit J Nutr 81:211–20
- ↑ Jump up to: 7.0 7.1 Hulshof KF et al. (1991) Diet and other life-style factors in high and low socio-economic groups (Dutch Nutrition Surveillance System) Eur J Clin Nutr 45:441–50
- ↑ Maillot M et al. (2007) Low energy density and high nutritional quality are each associated with higher diet costs in French adults Am J Clin Nutr 86:690–6
- ↑ Drewnowski A (1998) Energy density, palatability, and satiety: implications for weight control Nutrition Rev 56:347–53
- ↑ Rose D, Richards R (2004) Food store access and household fruit and vegetable use among participants in the US Food Stamp Program Public Health Nutrition 7:1081–8
- ↑ Jump up to: 11.0 11.1 Wardle J et al. (2000) Nutrition knowledge and food intake Appetite 34:269–75
- ↑ Prentice A, Poppit S (1996) Importance of energy density and macronutrients in the regulation of energy intake Int J Obes Relat Metab Disord 20:18-23 PMID 8646267
- ↑ Rolls B et al. (1998) Volume of foods consumed affects satiety in men Am J Clin Nutr 67:1170–7 PMID 9625090
- ↑ Prentice, A, Jebb, S (2003) Fast foods, energy density and obesity: a possible mechanistic link Obesity Rev 4:187-94 PMID 14649369
- ↑ Drewnowski A (1998) Energy density, palatability, and satiety: implications for weight control Nutr Rev 56:347–53 PMID 9884582
- ↑ Drewnowski A, Specter S (2004) Poverty and obesity: the role of energy density and energy costs Am J Clin Nutr 79:6-16 PMID 14684391
- ↑ Birch L (1999) Development of food preferences Annu Rev Nutr 19:41–62 PMID 10448516
- ↑ Jump up to: 18.0 18.1 18.2 Drewnowski A, Darmon N (2005) The economics of obesity: dietary energy density and energy cost Am J Clin Nutr 82:265S-73S
- ↑ Jump up to: 19.0 19.1 19.2 Drewnowski A et al. (2004) "Replacing fats and sweets with vegetables and fruits - A question of cost Am J Public Health 94: 1555-1559
- ↑ French SA (2003) Pricing effects on food choices J Nutr 133:841S-3S
- ↑ Jump up to: 21.0 21.1 Gordon-Larsen P et al. (2011) An economic analysis of community-level fast food prices and individual-level fast food intake: A longitudinal study Health & place 17:1235-41
- ↑ Powell, LM, Chaloupka FJ (2009) Food prices and obesity: evidence and policy implications for taxes and subsidies Milbank Quarterly 87: 229-257
- ↑ Schroeter C et al. (2008) Determining the impact of food price and income changes on body weight J Health Economics 27: 45-68
- ↑ Jump up to: 24.0 24.1 Darmon N, Ferguson EL et al. (2002) A cost constraint alone has adverse effects on food selection and nutrient density: An analysis of human diets by linear programming J Nutr 132:3764-71